Pelvic Organ Prolapse and Outlet Obstruction Constipation
Pelvic organ prolapse (POP) is a condition that can significantly impact a woman's quality of life. It occurs when the pelvic organs, such as the bladder, uterus, or rectum, descend from their normal positions and press against the vaginal walls. While POP is commonly associated with discomfort and urinary symptoms, it can also have an unexpected impact on another area: the digestive system. In this article, we'll explore how pelvic organ prolapse can lead to outlet obstruction and contribute to constipation.
Understanding Pelvic Organ Prolapse
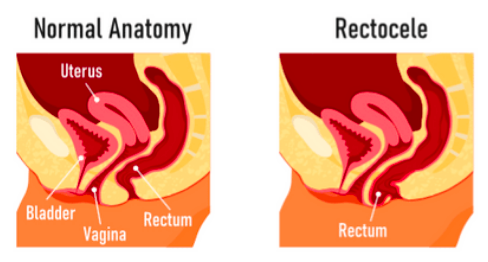
Pelvic organ prolapse occurs when the muscles and ligaments that support the pelvic organs weaken, causing them to shift downward. Depending on the specific organs involved, different types of prolapse can occur, including bladder (cystocele), uterine, and rectal (rectocele) prolapse. While the exact causes can vary, factors such as childbirth, ageing, hormonal changes, and genetics can contribute to the development of POP.
The Link Between Pelvic Organ Prolapse and Constipation
One lesser-known consequence of pelvic organ prolapse is its potential to cause outlet obstruction and contribute to constipation. When the organs, such as the rectum, descend from their normal positions, they can create an anatomical blockage in the pelvic region. This obstruction can hinder the normal flow of stool through the rectum and into the anal canal, leading to difficulties in passing stools.
Impact on Pelvic Floor Muscles
In addition to the physical obstruction caused by prolapse, the weakening of the pelvic floor muscles also plays a role in constipation. The pelvic floor muscles help support the rectum and contribute to proper bowel movements. When these muscles become compromised due to POP, they may struggle to coordinate effectively during defecation, resulting in inefficient evacuation and constipation.
Symptoms of Outlet Obstruction Constipation
The combination of pelvic organ prolapse and outlet obstruction can lead to several symptoms related to constipation, including:
- Straining: The need to exert excessive effort during bowel movements.
- Incomplete Evacuation: Feeling as if the bowel movement is not complete even after multiple attempts.
- Abdominal Discomfort: Experiencing discomfort or pain in the lower abdomen during or after defecation.
- Hard Stools: Passing dry and hard stools that are difficult to eliminate despite adequate fluid and fibre intake.
Managing Outlet Obstruction Constipation Due to POP
If you suspect that your constipation is linked to pelvic organ prolapse, there are steps you can take to manage the situation. The first step is to get an assessment by a pelvic floor physiotherapist
1. Pelvic Floor Exercises: Engaging in pelvic floor strengthening exercises, as guided by a pelvic floor physio, can help improve muscle coordination and support the affected organs.
2. Diet and Hydration: Consuming a fibre rich diet and staying well-hydrated can promote regular bowel movements and soften stools.
3. Positioning: Maintaining the proper squatting position during defecation can facilitate smoother stool passage and relieve strain on the pelvic floor.
4. Using a Support pessary: A vaginal support pessary can help to support the anatomy in a better alignment and therefore help with positioning to empty the rectum.

Pelvic organ prolapse can have far-reaching effects, even beyond the realm of urinary symptoms. The link between POP and outlet obstruction constipation highlights the intricate relationship between the pelvic organs and the digestive system. Recognising these connections and seeking professional guidance can pave the way to effective management and improved well-being.






